Dunedin Hospital’s Surgical Assessment Unit Fully Operational in Otago-Southland
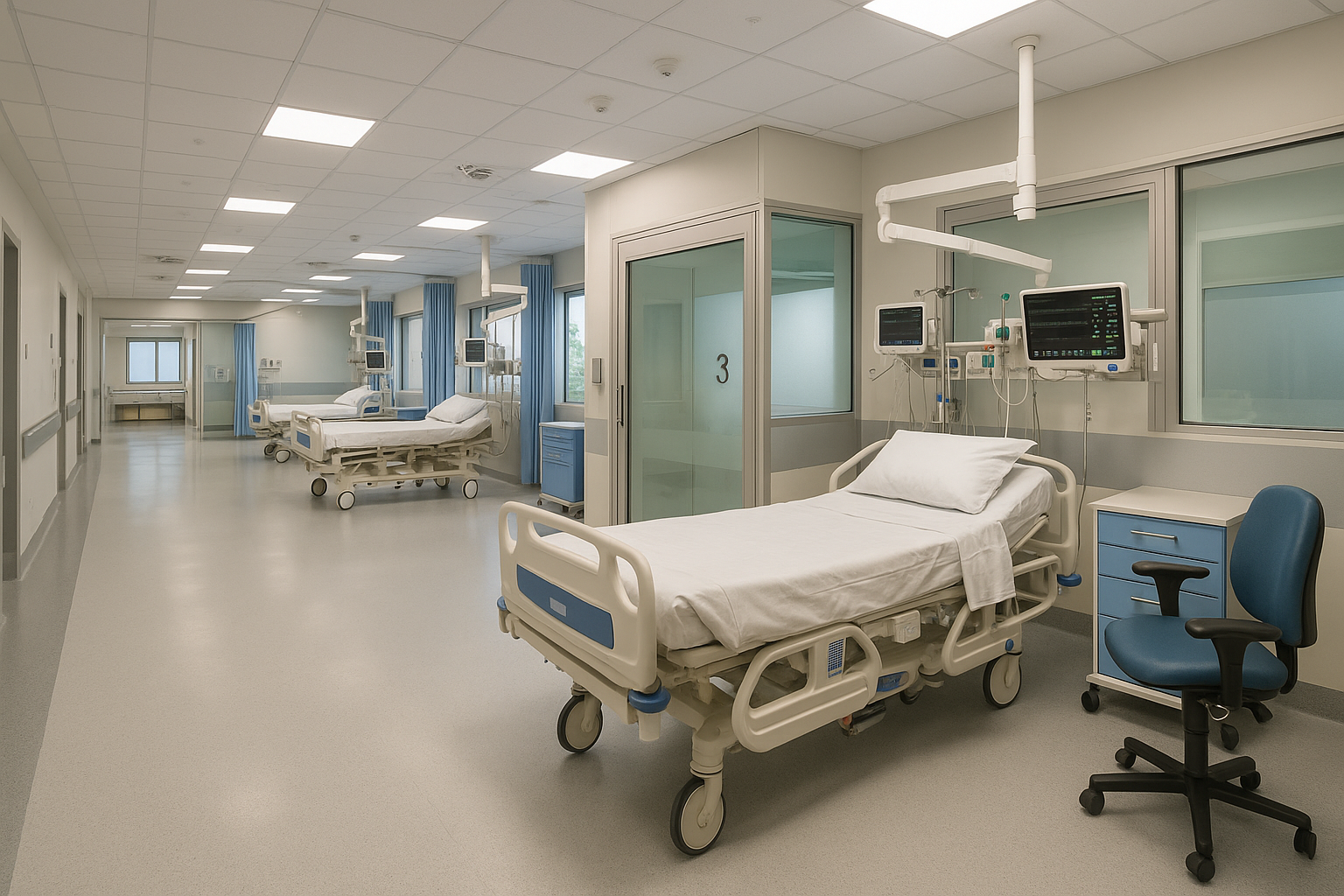
The SAU provides a dedicated clinical environment for patients presenting with acute surgical conditions such as appendicitis, abscesses, gallbladder issues, and other urgent but non-trauma cases.
- Country:
- New Zealand
A major step forward in acute surgical care delivery has been achieved with the full rollout of Dunedin Hospital’s new Surgical Assessment Unit (SAU), a purpose-built facility already transforming how patients are assessed, diagnosed, and treated across the Otago and Southland regions.
Health Minister Simeon Brown confirmed the $2.4 million unit is now fully operational, marking a shift toward faster, more targeted care pathways that reduce pressure on emergency departments while improving patient outcomes.
“This is about getting patients the right care, in the right place, at the right time,” Mr Brown said. “The Surgical Assessment Unit is already delivering faster diagnosis, earlier treatment, and significantly improved patient flow across the hospital.”
Designed for Speed, Precision, and Patient Comfort
The SAU provides a dedicated clinical environment for patients presenting with acute surgical conditions such as appendicitis, abscesses, gallbladder issues, and other urgent but non-trauma cases.
Unlike traditional emergency department pathways, patients can now:
-
Be referred directly by GPs, bypassing ED queues entirely
-
Be transferred rapidly from ED for specialist surgical assessment
-
Receive early intervention, including pain management, IV fluids, imaging, and diagnostics
This streamlined pathway ensures patients are assessed by surgical teams sooner, reducing delays that can impact outcomes.
“Patients no longer need to wait in busy emergency departments for surgical review,” Mr Brown said. “They are seen earlier in a calmer, purpose-designed environment, which improves both clinical care and patient experience.”
Strong Early Results from Pilot Phase
The SAU was initially trialled in December 2025 with just three beds. Since then, it has rapidly demonstrated its effectiveness:
-
More than 630 patients treated during the pilot phase
-
Significant reductions in time to assessment and diagnosis
-
Faster initiation of treatment plans
-
Consistently positive patient feedback
Following this success, the unit has now expanded to include six beds and five reclining treatment chairs, enabling greater capacity and flexibility in managing patient flow.
24/7 Operations Driving Faster Outcomes
Operating around the clock, the SAU ensures continuous access to surgical expertise — a critical factor in managing time-sensitive conditions.
Patients benefit from:
-
Immediate clinical assessment upon arrival
-
Faster access to diagnostic imaging and laboratory tests
-
Earlier decisions on whether surgery or admission is required
Importantly, the model supports rapid discharge where appropriate. Patients who do not require surgery or inpatient care can return home sooner with a clear treatment and follow-up plan, reducing unnecessary hospital stays.
Nurse-Led Model Enhances Efficiency
A standout feature of the SAU is its nurse-led care model, designed to maximise efficiency while maintaining high clinical standards.
The unit is staffed by:
-
Highly experienced surgical nurses
-
Clinical Nurse Specialists (CNS)
-
Registered Nurses (RNs)
-
Supported by on-call surgical medical specialists
This structure allows for rapid triage, early clinical decision-making, and continuous patient monitoring, ensuring care begins immediately upon arrival.
“The nurse-led model ensures patients receive expert attention from the moment they enter the unit,” Mr Brown said. “It’s a modern, efficient approach that is proving highly effective.”
Reducing Pressure on Emergency Departments
One of the most immediate benefits of the SAU is its impact on emergency department capacity — a critical issue, particularly as hospitals prepare for increased winter demand.
By diverting appropriate patients away from ED:
-
Emergency wait times are reduced
-
ED staff can focus on critical and life-threatening cases
-
Overall hospital flow becomes more efficient
“This initiative directly supports our goal of reducing ED wait times,” Mr Brown said. “It ensures emergency departments are available for those who need them most, while surgical patients receive faster, more specialised care.”
A Model for Future Healthcare Delivery
Health officials say the SAU represents a broader shift toward smarter, patient-centred hospital design — where specialised units streamline care pathways and improve system-wide efficiency.
The success of the Dunedin SAU could inform similar models across New Zealand, particularly in regions facing increasing demand on acute services.
“We are focused on practical solutions that deliver real results for patients,” Mr Brown said. “The Surgical Assessment Unit is a clear example of how targeted investment can improve care delivery, reduce delays, and enhance patient experience.”
Winter Preparedness and Long-Term Impact
With winter approaching — a period traditionally associated with increased hospital admissions — the SAU is expected to play a crucial role in maintaining service performance.
By enabling faster treatment and reducing unnecessary admissions, the unit strengthens the hospital’s ability to manage seasonal surges while maintaining quality care standards.
“Initiatives like this put patients at the centre of care,” Mr Brown added. “They ensure people in Dunedin and across the region receive timely, effective treatment when they need it most.”
As healthcare systems worldwide grapple with rising demand, Dunedin Hospital’s Surgical Assessment Unit stands out as a practical, scalable innovation — delivering measurable improvements in speed, efficiency, and patient outcomes.










